
ME (myalgic encephalomyelitis, also known as ME/CFS) is a serious, chronic illness, often triggered by a viral infection. Around 400,000 people in the UK and millions worldwide are thought to be affected. Research has been greatly underfunded and little is known about the mechanisms involved in the illness. However, the DecodeME study, published in 2025, pointed to the involvement of the immune and nervous systems, and indicated that susceptibility to ME is partly genetic. (Details of other recent research undertaken by UK ME charities can be found here, here and here.)
Symptoms of ME are extensive and include an overwhelming flu-like feeling, pain in any part of the body (in some cases unrelieved even by morphine), muscle weakness and cognitive dysfunction. A classic, defining feature of ME is deterioration following any activity beyond the person’s limit, known as post-exertional malaise (PEM) or post-exertional neuroimmune exhaustion (PENE). Acute sensitivity to sensory stimulation – light, sound, touch, taste, smell and movement – is another common feature, and can be one of the greatest challenges in daily existence.
Those more mildly affected are able to maintain aspects of normal living, but at its most severe, ME has been compared to the final stages of a terminal illness. Among others, Dr. Nancy Klimas, researcher and clinician at the University of Miami, said in 2007 that ME patients “experience a level of disability equal to that of patients with late-stage AIDS and patients undergoing chemotherapy.”

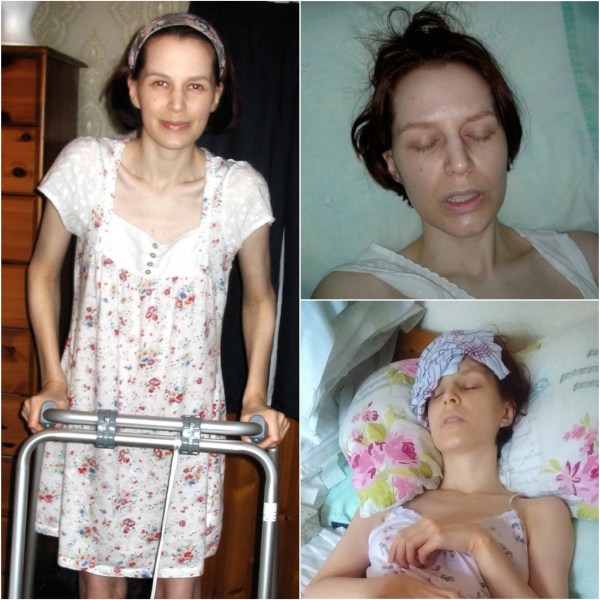
The most severely affected are completely bedridden and might require tube feeding, catheterisation and morphine. Sensitivities can be so acute that even the presence of another person in the room can cause a worsening of symptoms. A study in 2015 comparing 21 major illnesses, including heart disease and cancer, found that ME sufferers had the lowest quality of life by a significant degree. In some cases ME is fatal: the true death rate remains unknown, as death is often attributed to other causes.
There is no cure and no universally effective treatment. Recovery from severe ME is rare, but significant improvement is possible in some cases. However, this is generally dependent on the person receiving quality care and support, and living in an environment conducive to healing. Even then, progress is not guaranteed and usually represents a significant element of good fortune.
Since the 1980s, ME has also been known as chronic fatigue syndrome (CFS), but this name is unpopular with patient groups due to its trivialising nature. In addition the diagnostic criteria for CFS was historically much broader than for ME, meaning that ME became lost among more generalised fatiguing conditions. This had negative implications for medical research, as many studies purporting to investigate ME in fact included a spectrum of other conditions. Nowadays the condition is generally referred to as ME/CFS within the NHS and other official bodies.
For decades a prominent group of psychiatrists in the UK sought to reframe the illness as a psychological disorder requiring behavioural therapies. This has influenced healthcare policy around the world. The consequences for those with ME have been devastating, with many left irreparably worse through being forced into damaging treatments. Some families are subjected to care proceedings when professionals blame the parents for their child’s illness.
Many within the medical profession remain ignorant as to the severity of ME; others are openly hostile and dismissive. Even those who are sympathetic are often unable to respond to the complex needs of the most severely affected. The result is that some of the most seriously ill patients in society are left without anything resembling appropriate medical care.
In short, the illness itself forms only part of the burden experienced by those with ME: a major additional strain is coping with lack of awareness from professionals, the media and society in general. Even in the absence of a cure or effective treatment, the lives of those with ME would be transformed by more widespread understanding as to the true nature of the illness.
I have written in more detail about these issues here and here. And in The Power of Listening, a piece written for a training seminar for junior doctors, I describe the difference that can be made when professionals take the time to truly listen to their patients.
